Your experience of labour and birth should be just that — yours. Every birth is unique and each woman will approach childbirth in her own way. This article looks at options for women who choose to give birth without the use of medical pain relief.
Why do women avoid medical pain relief?
There are many reasons why you might choose to avoid medical pain relief. These may include:
* you would like to feel in control
* you are worried about having a negative reaction to medical pain relief – sickness, dizziness, etc
* you would like to experience labour
* you would like to feel your baby being born
* you are afraid of needles
* you would like to avoid a change of risk status (epidural changes your risk status from low to high risk)
* you would like to avoid increased risk of interventions
* you do not want to increase your risk of Caesarean section or assisted delivery
* you would like to move about freely in labour
* you would like to give birth in an upright position or off the bed
* you would like to labour or birth in water
* you would like access to midwife led care (MLU or DOMINO or homebirth)
* you want to avail of the early release home scheme
* you would like to avoid a catheter
* you would like to avoid continuous monitoring with CTG
* you would like to avoid drugs that cross the placenta to your baby
* you would like to breastfeed and are concerned pain medications interfere with the initiation of feeding
Your Birthing Environment
The environment you labour and birth in can have a strong influence on your overall birth experience and ability to cope. A birthing environment should be supportive, encouraging, and relaxed. Your brain reacts to stressful and clinical environments. Fear and resistance to what feels natural to you can cause your body to react as if it is in danger – a fight or flight response. If you experience an excessively stressful situation, your body reacts by charging up hormones, like adrenaline, to prepare your body to either stay and fight or to flee from the stressful environment you find yourself in. Once the fight or flight response is activated, your blood pressure and heart rate is raised. You have increased muscle tension. Your pupils dilate and you experience increased perspiration. If fight or flight is activated in labour, it is counter-productive to the environment you need to help your body relax and an inhibitor of oxytocin – making labour longer and more painful.
This fantastic video creatively looks at how environment plays an important part in how we labour.
Creating a Positive Birthing Environment
* Choose a birth partner who supports you and your birth choices
* Choose care options which suit you and your baby’s needs best. You can read more about care options here
* Carve out your own space in labour – labour wards can be busy places try to find a space that you and your partner feel relaxed in – in the shower or bath, go for a walk, explore the hospital grounds or garden, walk the stairs or corridor. If you cannot leave your ward find a way to make space in your own surroundings – draw the curtains and use ear phones to tune out noise. Watch a DVD.
* bring comforts with you – your own pillow, music, a comfy blanket, a heat pack
* have comfort foods and drinks prepared
* dim the lights
* ask for privacy – time on your own in labour or limiting who is in the room with you
“On my first pregnancy I had a long labour with an OP baby, and the hospital was very very busy. I discussed my desire to labour and birth without pain medications with the midwife on duty and she brought me to a private room with a deep bath. I laboured in there for hours in the warm water with just my husband. By the time she came to check me, I was well on my way to giving birth!”
Put on a Birthing Filter
We are bombarded by the tv, movies, soaps, and newspapers – all trying to out-do themselves to show birth as dramatic, dangerous, and painful. While this may seem harmless – you might not even think about it – these images and stories are being stored in your memory bank and to make up your internal belief system about how you feel about giving birth. If you only hear and see mostly negative stories and images of birth, this is likely to be your reality. While if you see and hear mostly positive images and stories of birth, you are reinforcing positive healthy birth as your reality.
In the last decade birth programs have become popular viewing on mainstream television. You may feel that watching these programs will prepare you for labour and birth. Unfortunately, many of these programs only highlight routine obstetric led practices and reinforce interventions which are not supported by evidence. These programs have a big part to play in how you view birth and reinforce that unnecessary interventions and practices that are not supported by evidence are normal and OK despite the increase in risks to you and your baby.
Horror stories serve no purpose to you in pregnancy. It is one person’s experience. They will not make you more informed. Surround yourself with positive birth stories and images during your pregnancy.
“The factor that best predicts a woman’s experience of labor pain is her level of confidence in her ability to cope with labor”(Lowe 2002).
Try to surround yourself with women with similar birth choices to support one another, bounce ideas off, rant to! Sometimes, especially if this is a first baby, women can feel alone, unsure, or overwhelmed in pregnancy. A strong support network with like-minded women can be extremely reassuring. Women supporting other women is invaluable. Seek out women whom have given birth without medical pain relief. Ask them to share their stories and any tips they may have.
TIP: Check out the Positive Irish Birth Stories on the 42 weeks website!
TENS Machine
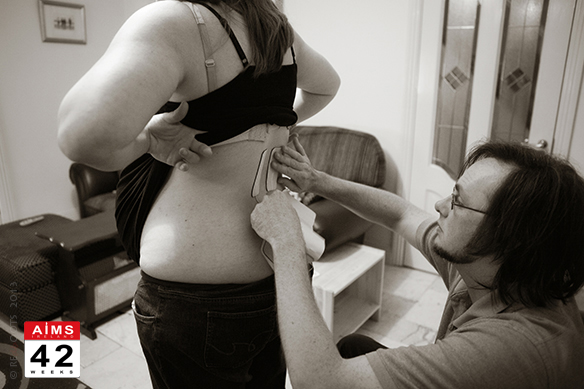
Each TENS comes with four sticky pads which you attach where you gain the most relief, usually on your lower back but they can also be applied to acupuncture points or directly to the head. The pads are connected to electrical leads which are attached to a control panel. It is possible to buy replacement pads for TENS machines so the devices can be reused, shared or rented. Control panels also often come with a belt clip and/or neck cord so you can secure the device to your clothing while moving around during labour.
You are in control of the TENS intensity. The hand-held controls allow you to start at a low intensity and increase intensity as your labour progresses. The TENS machine works by sending small electronic pulses through the machine to the leads and the pads which are attached to your skin. When using a TENS you will feel a ‘buzzing’ or ‘tingling’ feeling which can be increased from low to high intensity. An obstetric TENS machine, designed specifically for use during labour, will usually have a “boost” button on the control pad which you can press to temporarily increase the intensity of the pulses.
TENS is believed to change or suppress the way our brain receives signals of pain. The electrical pulses are thought to stimulate nerve pathways in the spinal cord which block the transmission of pain. You may find the TENS is a good distraction during labour. Many women find TENS helps them feel in control. TENS machines are thought to be most helpful in the early stages of labour, however, there is little evidence to suggest that TENS is an effective form of pain relief. Anecdotally, women report it being a good support or distraction to them if used from very early on in their labour.
TENS is not recommended if you have a pacemaker or epilepsy. It is not recommended to use over the uterus.
Advantages of TENS
- you are in control of when to use the TENS and intensity
- TENS acts as a distraction
- many women find TENS is effective in early labour
- you can move about freely while using the TENS
- you may use the TENS at home or if you decide to leave the maternity unit
- A TENS with a boost button offers you full control over the intensity of the device
- There is some evidence that women using TENS are less likely to rate their pain as severe but results were not consistent.
- Many women who have used a TENS during labour say they would be willing to use TENS again in a future labour.
Disadvantages of TENS
- you will need your partner to help you place the pads on your back
- you cannot use TENS in water – bath, shower, or birth pool
- you may need to remove the TENS if you have a CTG
- you may not find it is effective pain relief
- you may find the sensation irritating
It is worth noting that a Cochrane Review of the use of TENS during labour found that its use did not seem have an effect on the length of labour, interventions in labour, or the well-being of mothers and babies.
What women say . . .
“I used TENS on my first from the early stages (when pains were about 10-15 minutes apart) until I got to the hospital. I was 7cm on admission. I found TENS great and think it helped me stay home as long as I did”
And:
“I used TENS at home and found it grand for backache but not the pains in the front. When I got to hospital I had to take it off for the CTG anyhow”
And:
“I really didn’t like it – I found it frustrating trying to press buttons as I was having contractions and the sensations really annoyed me. I found it much easier to cope once I took it off and I could just focus on each contraction!
And:
“It was fantastic for pre-labour warm up that went on for days and for the car journey into hospital.”
References & Additional Reading:
TENS Machines – http://www.patient.co.uk/health/tens-machines
Cochrane Review: TENS (transcutaneous nerve stimulation) for pain relief in labour
Water Therapy, Water Immersion and Water Birth
Research has shown that while it is unknown if water actually removes pain, warm water can help you relax and many women report it to be a good form of managing pain in labour.
Water Immersion in Labour
Water immersion is where a woman’s abdomen is completely submerged in water, so this would refer to labouring in a deep bath or tub that is larger than the average domestic-sized bath or a purpose-made birth pool.
A Cochrane Review in water in labour and birth published in 2012 showed that water immersion during the first stage of labour significantly reduced the need for epidural or spinal analgesia, without adversely affecting the length of labour, instrumental and C-section delivery rates or neonatal wellbeing. One trial showed that immersion in water during the second stage of labour increased women’s reported satisfaction with their birth experience. The review also found that further research is needed to assess the effect of immersion in water on neonatal and maternal morbidity.
Advantages of Water Immersion
- the buoyancy of the water enables you to move more easily than on land
- water immersion may be associated with improved blood flow to the uterus, less painful contractions and a shorter labour
- you are less likely to have interventions during labour
- the ease of mobility may optimise foetal positioning
- increased maternal satisfaction and sense of control
- a comfortable temperature reduces blood pressure and promotes relaxation
Disadvantages of Water Immersion
- Women labouring in water may be asked to leave the water for the second stage (pushing stage) of labour. This also applies in hospital run homebirth schemes
- Care needs to be taken to ensure that the water is neither too hot or too cold. Some sources suggest that the water should be no hotter than 37 degrees centigrade while others suggest that the mother should be encouraged to regulate the temperature of the water to suit themselves
- Caregivers may feel that it is difficult to access the labouring woman when she is in labour although some may argue that it is this reason that leads to less interventions during the birth process
- Due to the small number of birth pools available in a maternity unit setting, the pool may be in use when you would like to use it
- Usually, water immersion in a hospital setting is only offered to low risk women
In a 2011 survey, AIMS Ireland asked:
“Do you think women should have access to water for pain relief during labour in Irish maternity units?”
Results: YES = 99.0% – NO = 1.0% – I DON’T KNOW = 0.0%” AIMS Ireland Waterbirth Survey Results (2011)
AND:
“Would you like to have the option of having a waterbirth in a birth pool available to you?”
Results: YES= 91.0% – NO = 5.0% – I DON’T KNOW = 4.0% ” AIMS Ireland Waterbirth Survey Results (2011)
Accessing Water for use in labour in Ireland
Only a handful of maternity units in Ireland have birthing pools, namely The Coombe, Cork University Maternity Hospital, the Our Lady of Lourdes MLU and the Cavan MLU. There is a birth pool in Waterford Regional Hospital which hasn’t opened to date. Some have access to deep baths, while others only have showers.
If you are having a homebirth, you will need to source an inflatable birth pool. These are available new or second hand from mothers selling them on. You may even be able to borrow one!
You may wish to purchase or borrow a birth pool to labour in at home – even if you are having a hospital birth! Many mums contacting AIMS Ireland have found this an effective way to stay at home as long as possible and avoid routine intervention including medical pain relief!
What Women Say . . .
Would have much preferred to stay in water for at least the full labour if not for the birth. I feel that I wouldn’t have used an epidural had I been able to stay in the water.
AND:
On first an amazing foreign midwife suggested I use it – I was in early labour on an OP baby. The minute I got in the water I felt more relaxed and in control. Spent ages in the bath and it was fantastic! Unfortunately I got out later and lost the bath – found it a huge difference without the water. When the bath did become available again my new midwife wasn’t keen and I didn’t think to make an issue of it – her being the professional and all. Felt much more intense and out of control without it.
AND:
I laboured in a bath in a Dublin maternity hospital. I was progressing very well and found it very difficult to get out when I felt I had to.
AND:
I used the shower for hours during my first labour. I hated coming out of it for checks
Waterbirth
As mentioned above, despite 92% of respondents to the AIMS Ireland survey thinking women should have access to waterbirth in Irish maternity units, it is NOT an option available in MOST of Ireland’s maternity units. In the majority of units if you use the pool/bath or shower for labour, you will be asked to come out for the birth of your baby. Currently (March 2017) the Coombe hospital are celebrating 100 water births. Water births are also available in the MLUs in Cavan and OLOL and of course at home with HSE home birth midwives and Private Midwives
If you would like a waterbirth, be sure to speak to your Health Care Providers about your options.
What women say . . .
I feel it is such a shame that my local hospital has a birthing pool but we are not allowed to give birth in it. I am aware a baby died during a waterbirth years ago. Does this mean that there cannot be another waterbirth in an Irish hospital for all eternity ? I am pregnant with my third and last baby so a waterbirth option is now gone for me
And:
I cannot understand why waterbirths are not an options in all maternity units. It cannot be because of a tragedy of a baby dying after being born surely, because these tragedies happen all the time regardless of where and how babies are born
For moreinformation on uusing a pool at home go to http://homebirthireland.com/using-a-birth-pool-for-labour-or-birth-at-home/
References:
AIMS Ireland Waterbirth Survey 2011
Cochrane Review: Immersion in water in labour and birth
RCOG and RCM Joint Statement on Water During Labour and Birth
Using A Doula
You are probably thinking – How can a person be pain relief?!? But the concept of doulas has been around for centuries.
The desire to have our mothers, sisters or female friends with us in labour is a primal and instinctual example of women’s abilities to act on intuition. For centuries women have given birth with the support and understanding of elder women who have the life experience to guide the labouring woman through her birth. It makes absolute sense that women would chose to labour with their mother or sister in addition to their husband or partner. Women are naturally empathetic, supportive and strong. Many have the experience of having birthed themselves, which can add another dimension to support.
Research has shown that the use of a doulas is extremely beneficial for the labouring woman. According to some research, midwives and nurses are only able to give 10% of their time in ‘supportive roles’ in labour and birth. It is not surprising then that women feel the need to find additional emotional support either in a family member, friend or through hiring a doula.
Research has found that women who laboured and birthed with a female partner experienced extensive benefits to those who did not. Women had more spontaneous vaginal deliveries (91% to 71%), less analgesia use during labour (53% to 73%), less synthetic oxytocin (13% to 30%), fewer amniotomies (waters broken) to augment labour (30% to 54%), fewer vacuum extractions (4% to 16%) and fewer Caesarean sections (6% to 13%) compared to the control group. The support of a female relative while in labour is shown to have fewer interventions and increased frequency of normal vaginal deliveries.
“If a doula were a drug, it would be unethical not to use it.” ~ John H. Kennell, MD
What’s a Doula?
Doula (Greek) is a woman experienced in childbirth who provides continuous emotional support to the labouring mother and her partner. A doula’s primary role is to the mother. Their sole focus is on the emotional wellbeing of the woman in labour. Unlike a midwife who may be assigned several labouring women and whose focus in on physiological/medical birth issues, the doula’s primary focus is on one woman and is undivided emotional support. This support is reflected in the doula ideology and doula promises.
Research has shown that due to the individual emotional support provided that women labouring with a doula may prosper from a range of benefits.
Evidenced Based Benefits
Research shows that:
· women using a doula have a 50% reduction rate in Caesarean section
· women using a doula have a 40% reduction in the rate of forceps deliveries
· women using a doula have a 60% reduction in request for the epidural
· women who used a doula had a decrease in labour length by 25%
A doula does not replace your partner but rather encourages him or her to be as involved as his/her comfort level allows.
“My husband wasn’t initially sure about using a doula but on the day he found it a great relief to have her there. It meant he could go through this with me – he could have his own experience knowing that my doula would provide all the emotional support I needed. It took the pressure off of him – he was really worried about how he would perform on the day.”
Promises of a Doula
1. You cannot hurt my feelings in labour
2. I won’t lie to you in labour
3. I will do everything in my power so you do not suffer
4. I will help you feel safe
5. I cannot speak for you but I will make sure that you have a voice and I will make sure you are heard
What Women Say . . .
“on my first labour I felt quite alone. The midwife was busy writing notes and my husband tried but just didn’t quite know what to do. He felt stressed with the pressure and was emotionally involved himself. On my next baby we decided to hire a doula. I met with her over my pregnancy so we really felt comfortable with her by the time I went into labour. In labour, it was brilliant, she was relaxed and it rubbed off on me. Her experience really shown through and her suggestions really helped get me through.”
And:
“After I had my own babies I decided to train as a doula. It is such an honour to support a woman through her labour.”
And:
“I always loved the idea of having a friend or a doula with me in labour but I am quiet self conscious and worried about having someone seeing me undressed or being vocal. I had a talk about it with my friend, who has been a doula before, and we came up with a plan and the promise that if I changed my mind at any time it was OK, no hard feelings. In the end, I was so happy she was there. I felt so loved and cared for – by my husband and my doula. It was a beautiful birth. “
How do I find a doula?
You can find a doula in Ireland through the following websites. A word of mouth recommendation is also another good option. It’s a good idea to speak or meet with a number of doulas so that you can find the right one for you.
You might try The Irish Doula Directory or various other doula directories
What is the policy in Irish hospitals when you have a doula – I’ve heard they’re not allowed in with your birth partner?
Policies differ from unit to unit. Often maternity hospitals state that only one birth partner is allowed to be present with a labouring woman. However, the vast majority of hospitals are happy to approve the presence of both your birth partner and your doula if you communicate in writing with them in advance. A letter to the director of midwifery and occasionally a meeting in person will usually ensure that your doula has permission to attend your birth. The Coombe maternity hospital in Dublin recently relaxed their policy on the attendance of doulas at births. Women who plan to have a doula when attending the Coombe don’t even need to have it noted in their file at one of their antenatal appointments.
 AIMS Ireland
AIMS Ireland